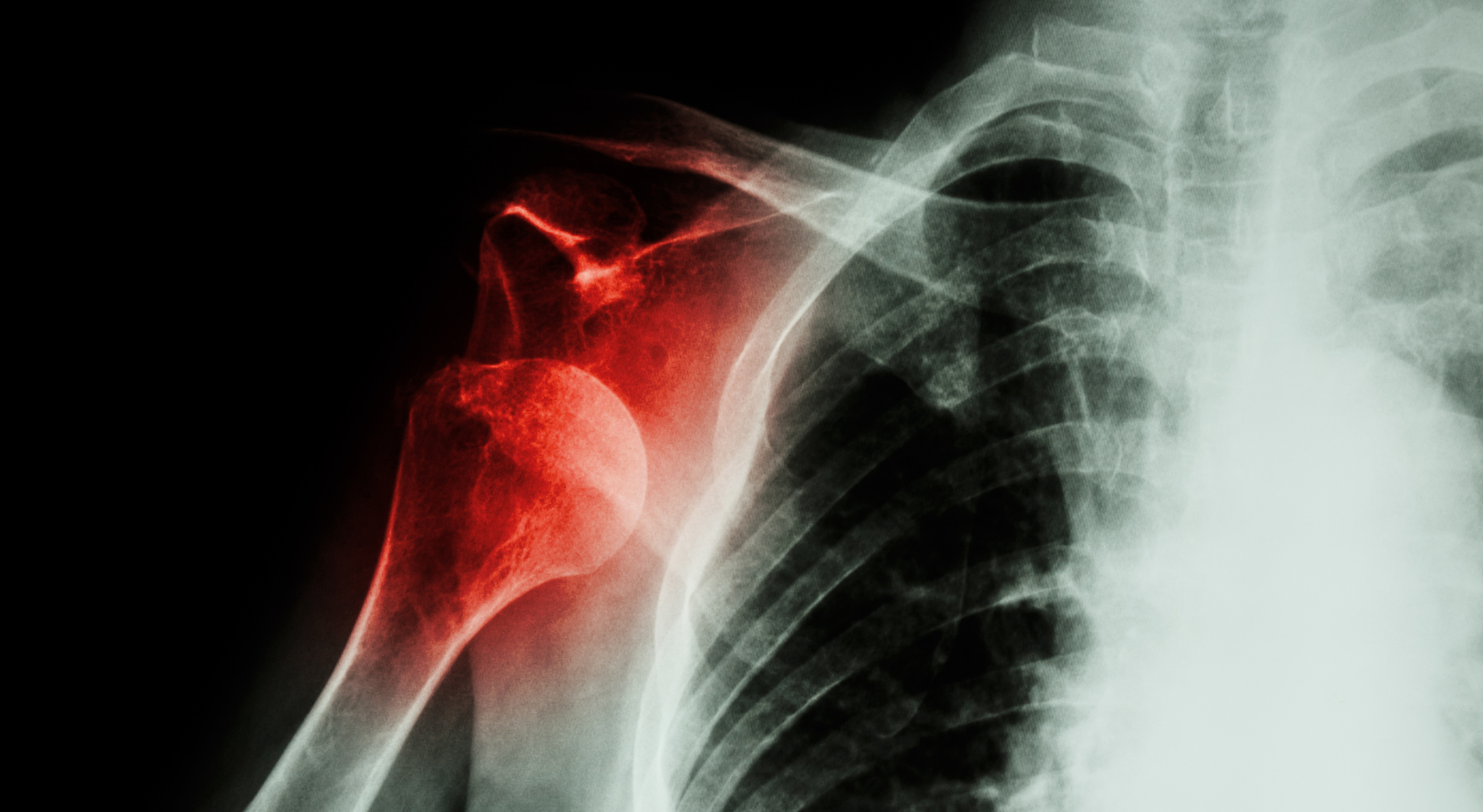
Shoulder instability is a condition in which the components of the joint, specifically the humeral head and the glenoid socket, are improperly aligned. Temporary, partial displacement of the humeral head relative to the glenoid socket is referred to as subluxation, while complete, temporary or permanent displacement is referred to as dislocation. Initially, shoulder instability often occurs as a result of direct trauma. However, it can also occur secondarily as a result of recurrent subluxations or dislocations.
The most common cause of shoulder dislocation is direct trauma, which applies a force that displaces the humeral head from the glenoid socket. The humeral head usually relocates towards the front and downward in relation to the glenoid socket. Posterior dislocations are much rarer and occur as a result of a fall onto the shoulder or from a collision in contact sports.
There are also cases of spontaneous shoulder dislocation without any traumatic event, which are more common in individuals with joint laxity. Joint laxity is characterized by a loose ligamentous and tendinous apparatus. Repetitive overhead motions in sports such as swimming, tennis, and volleyball can also contribute to shoulder instability. Additionally, it can occur in individuals with connective tissue disorders.
As a result of direct trauma or repetitive micro-trauma and constant subluxation of the joint, both soft tissue and bony structures can be damaged. These include: damage to the cartilage, damage to the rotator cuff, damage to the joint capsule, labral tears, Hill-Sachs fracture (typical fracture of the humeral head), and damage to the key stabilizing structure, which is the glenoid labrum and the glenoid rim. Damage to these last two structures and their healing in an abnormal position will result in shoulder instability.
Symptoms of shoulder instability
Characteristic symptoms of shoulder instability include: a feeling of slipping, dislocation of the joint, sometimes accompanied by pain, a sense of increased range of motion, apprehension with certain movements, and joint instability.
In the case of acute, traumatic episodes, symptoms include: severe pain, shoulder deformity, audible popping or snapping, subluxation, loss of mobility/joint locking, and often numbness in the limb.
Diagnosis
The diagnosis of shoulder instability is based on a clinical examination conducted by a doctor who assesses symptoms and determines the degree and type of joint instability through tests. The medical history is also important in determining whether conservative or surgical treatment is appropriate.
Additional diagnostic tests include:
- X-ray (radiograph) – provides an initial assessment of the bone structures and the presence of fresh fractures, particularly in the glenoid socket of the shoulder joint.
- Magnetic resonance imaging (MRI) – allows for evaluation of intra-articular injuries, including labral tears, most commonly anterior labral tears or labral tears combined with glenoid rim fractures, known as Bankart or bony Bankart lesions. Contrast-enhanced MRI can provide a clearer image.
- Computed tomography (CT) – used to accurately evaluate bony structures and the extent of glenoid socket loss in chronic shoulder instability.
Treatment for shoulder instability
Acute traumatic shoulder dislocation requires immediate medical attention for joint reduction. X-rays are initially performed to assess bone structures and determine the type of dislocation. Joint reduction is performed under local anesthesia and analgesics are administered for pain relief.
After reduction, a repeat X-ray is recommended. The patient is immobilized in a brace for 2-3 weeks. Subsequently, rehabilitation is recommended to improve muscle function and joint stability.
In cases where attempts to reduce the shoulder joint in an outpatient setting are unsuccessful, it may be necessary to perform the reduction under general anesthesia. If this attempt fails as well, the patient is then qualified for surgical reduction of the joint.
For first-time dislocations in individuals who do not engage in high-level sports or in older individuals, conservative treatment is the initial approach. This involves initial immobilization and rehabilitation.
Modifying training and rehabilitation is also recommended for individuals with the above-mentioned joint laxity to increase control and stability of the shoulder joint and shoulder girdle. Only in cases of no improvement and persistent symptoms, surgical treatment is considered.
The type of procedure depends on the indications for surgery, with arthroscopic treatment being the standard procedure. The surgery involves debriding and refreshing the damaged area, mobilizing, and ultimately, stabilizing the damaged labrum to the glenoid socket using specialized anchors and sutures.
The procedure lasts approximately 90-120 minutes, depending on the extent of the damage. After surgery, the limb is immobilized in a brace for about 4 weeks. Basic rehabilitation can begin as early as the second week post-surgery. Return to work usually occurs after about 4 weeks. Rehabilitation and a return to full sports activity take about 8 months.
In cases of joint laxity, the surgery involves tightening and shrinking the joint capsule along with the labrum-ligament complex. This procedure requires postoperative rehabilitation and muscle stabilization. However, it is important to note that despite treatment, there may be a recurrence of symptoms and a return to the initial state.
In cases where the initial stabilization of the labrum fails or in cases of damage to the anterior rim of the glenoid socket, a Laterjet procedure may be necessary. This procedure involves increasing the anterior-posterior dimension of the glenoid socket by transferring a bone fragment from the coracoid process, which is located near the shoulder joint. The harvested bone fragment is then stabilized on the previously prepared anterior rim of the glenoid socket using two screws or special suture/tape implants, secured with small titanium plates in the front and back of the socket. Finally, the labrum is stabilized using anchors.
This surgery can be performed fully arthroscopically or with an open approach, with an incision of approximately 8 cm on the anterior surface of the joint.
Postoperative management includes stabilization in a brace for about 4-6 weeks. Rehabilitation is initiated during this time. Return to daily activities takes about 6-8 weeks, while a return to full sports activity may take around 12 months.
The shoulder area in MIRAI is managed by:
Bartosz Dominik – material development for the website
Michał Drwięga
Welcome!